Intra-articular and PRP Injection
Intra-articular injection is a type of injection administered directly into the joint to relieve pain. This treatment is used for inflammatory joint conditions such as rheumatoid arthritis, psoriatic arthritis, gout, tendinitis, bursitis, carpal tunnel syndrome, and sometimes osteoarthritis.
Common substances injected into the joint for this purpose include corticosteroids (steroids), local anesthetics, hyaluronic acid, Botox, and regenerative medical injections such as platelet-rich plasma (PRP), stem cells, and prolotherapy. These aim to relieve pain and stimulate the healing of cells and tissues.
What is PRP?
Platelet-rich plasma (PRP), sometimes called therapeutic PRP or autologous conditioned plasma (ACP) therapy, aims to use the natural healing properties of blood to repair damaged cartilage, tendons, ligaments, muscles, or even bone. Many people turn to PRP injections to treat a wide range of orthopedic conditions, including osteoarthritis. It is most commonly used for knee osteoarthritis but can be applied to other joints as well.
When treating osteoarthritis with PRP, the doctor injects PRP directly into the affected joint. The goals are to:
Reduce pain
Improve joint function
Potentially slow, halt, or even repair cartilage damage
PRP is obtained from the patient’s own blood. Therapeutic injections contain plasma with a higher concentration of platelets than normal blood.
To better understand PRP therapy, let’s answer a few questions:
What is plasma?
Plasma is the liquid component of blood. It serves as a medium for red and white blood cells and other substances circulating in the bloodstream. Plasma is mostly water but also contains proteins, nutrients, glucose, antibodies, and other components.
What are platelets?
Like red and white blood cells, platelets are a natural component of blood. Platelets themselves do not have inherent healing properties; rather, they secrete growth factors and other proteins that regulate cell division, stimulate tissue regeneration, and promote healing. Platelets also help with blood clotting. Individuals with defective or low platelets may experience excessive bleeding from minor cuts.
How is platelet-rich plasma (PRP) prepared?
The most common method for preparing PRP involves centrifuging a sample of the patient’s blood. A vial of blood is placed in a centrifuge and spun at high speed. This separates the blood into multiple layers. Once centrifugation is complete, the doctor removes the vial and prepares the PRP solution for injection.
Benefits of PRP Therapy:
PRP is autologous, meaning it comes from the patient’s own body, so it is natural and carries minimal risk of adverse reactions.
Other treatments for mild to moderate osteoarthritis can be inconsistent, vary from person to person, or have side effects:
Exercise can improve symptoms but does not always eliminate them.
Cortisone injections can reduce osteoarthritis pain, but repeated injections may weaken ligaments and tendons over time and may negatively affect healthy cartilage.
Anti-inflammatory drugs (NSAIDs) such as aspirin and ibuprofen can relieve pain, but long-term use may worsen stomach, blood pressure, and heart problems.
Joint replacement surgeries are major procedures that require long-term rehabilitation and are usually reserved for more disabling arthritis cases.
Patients should remember that PRP is not a complete cure and is best used in combination with non-surgical treatments and lifestyle modifications such as physiotherapy, weight loss, braces, and NSAIDs.
Contraindications for PRP:
PRP injections may not be suitable for osteoarthritis patients who:
Have a medical condition that could worsen or spread with injection, such as active infection, metastatic disease, certain skin disorders, blood disorders, or bleeding problems.
Are on anticoagulant therapy and cannot temporarily pause treatment.
Are anemic.
Are pregnant.
Additionally, patients with allergies to bovine products should inform their doctor. PRP sometimes contains an additive called bovine thrombin, which may trigger allergic reactions in these patients.
PRP injection requires precision, as it must be administered directly into the joint capsule. Therefore, an experienced physician should perform the injection. At Dr. Ali Moazami Pour’s clinic, we ensure this is done safely and professionally.
Precautions Before Injection:
Avoid corticosteroids 2–3 weeks before the procedure.
Stop taking NSAIDs (e.g., aspirin, ibuprofen) or arthritis medications like Celebrex one week before the procedure.
Stop anticoagulants five days prior to the procedure.
Drink plenty of fluids the day before the procedure.
Some patients may need anti-anxiety medication immediately before the procedure.
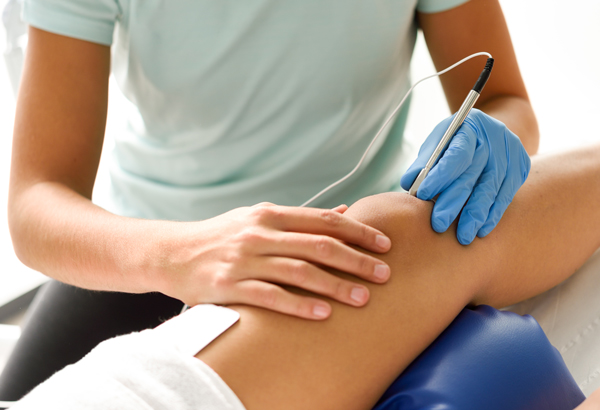
Step-by-step platelet-rich plasma injection
PRP injection is an outpatient procedure that involves blood collection, PRP preparation, and injection, typically taking 45 to 90 minutes.
Blood is drawn from the patient’s arm vein into a vial (usually 15 to 50 mL).
The blood is processed using a centrifuge.
The doctor prepares the centrifuged platelet-rich plasma for injection.
The injured joint area is disinfected with antiseptic agents such as alcohol or iodine.
The patient is asked to rest, which facilitates the injection and can also help reduce injection pain.
The doctor injects a small amount of platelet-rich plasma (often only 3 to 6 mL) into the joint capsule using a syringe and needle.
The injection site is cleaned and bandaged.
PRP usually triggers a series of biological responses, and the injection area may be swollen and painful for about 3 days.
Post-PRP Injection: Immediate Follow-Up Care
Patients should avoid heavy activities and putting stress on the treated joint for several days.
Do not take anti-inflammatory medications; an alternative pain reliever may be prescribed by the doctor.
Use a brace or band to protect and immobilize the treated joint. Patients receiving injections in the ankle, knee, or hip may be advised to use a cane.
To help reduce pain and swelling, apply a cold compress several times a day for 10 to 20 minutes.
Patients without physically demanding jobs can usually return to work the next day. Normal activities may typically resume a few days after the injection once swelling and pain decrease. Do not resume anti-inflammatory medications until cleared by the doctor.
Physiotherapy:
If the injection successfully reduces the patient’s pain, physiotherapy will likely be prescribed. Simple exercises to build and maintain muscle strength around the treated joint help reduce arthritis symptoms and can slow or halt further joint degeneration.
